VOLUME 27, ISSUE 2 • JUNE 2023 Full issue »
VOLUME 27, ISSUE 2 • JUNE 2023 Full issue »

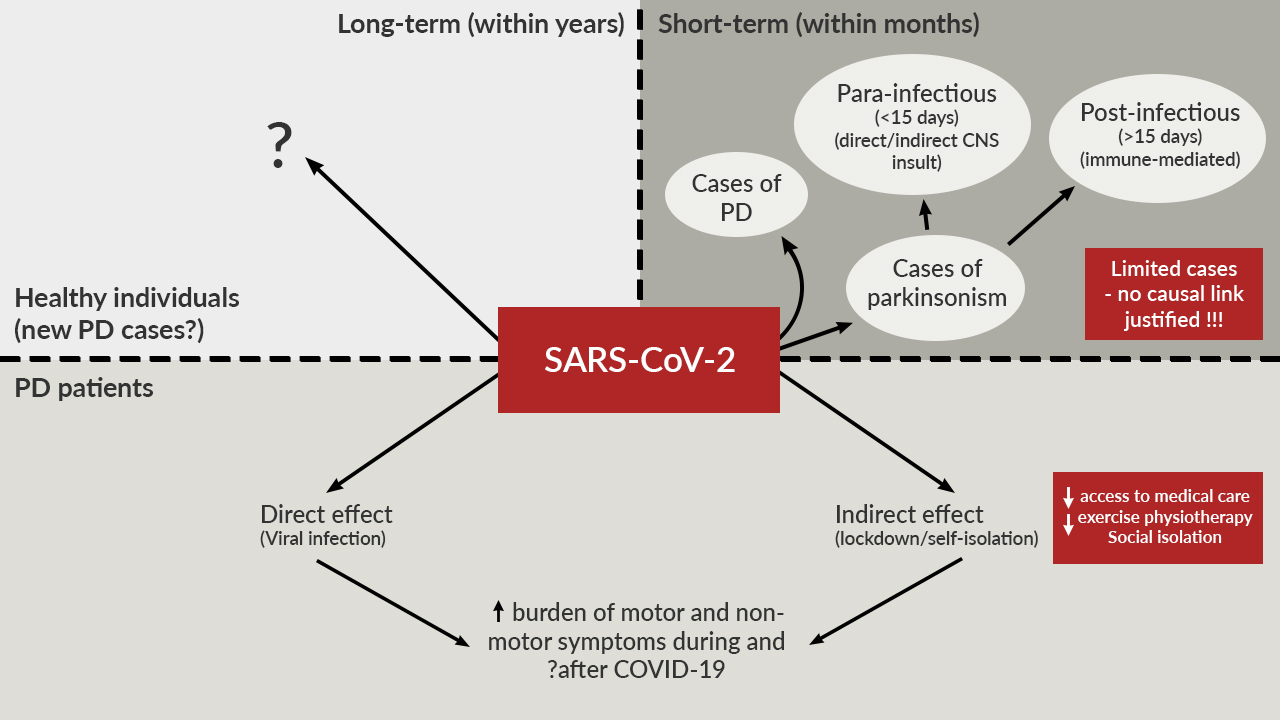
The description of post-encephalitic parkinsonism temporally linked to the 1918 influenza epidemic, combined with the growing awareness that movement disorders secondary to viral infectious are not infrequent, have underpinned reports of parkinsonism and other movement disorders following a confirmed SARS-CoV-2 infection. In a recent review, we have summarized the current evidence on parkinsonism with a presumed viral origin, focusing on potential pathophysiological mechanisms (para-infectious versus post-infectious) and clinical features [1]. We have also described the role of viral infections as a risk factor for Parkinson’s disease (PD) development, with a focus on SARS-CoV-2 [1]. Initial observations suggested that SARS-CoV-2 infection could lead to the emergence of new cases of parkinsonism or PD in susceptible individuals. In our recent review, we have presented such reported cases and discussed potential underlying mechanisms, concluding that available data cannot yet justify a clear link between the Coronavirus disease 2019 (COVID-19) pandemic and a subsequent parkinsonism wave [2]. On May 5, 2023, the World Health Organization announced that COVID-19 no longer constitutes a public health emergency of international concern; however, since selected viral infections have been found to increase the risk for PD occurrence [1], vigilance for the emergence of PD in well-characterized cohorts of patients with COVID-19 is warranted and is currently in progress, such as in the COVID-19 Clinical Neuroscience Study (COVID-CNS) in the United Kingdom.
We have also contributed to signpost the potential acute and long-term implications of COVID-19 in patients with PD, publishing the first multicenter and international case series on these topics [3, 4]. While acute implications of SARS-CoV-2 infection in PD, including worsening of motor and non-motor features, have been reported in several studies, evidence on long-term sequelae of COVID-19 in PD is limited [5]. We observed that the post-COVID-19 syndrome in PD is characterized by worsening of motor symptoms, fatigue, cognitive and sleep disturbances [4], a profile similar to the published description of long COVID in the general population. Whether this is due to the direct effects of SARS-CoV-2 infection or to its indirect effects, namely the effect of a prolonged lockdown leading to social isolation and reduced access to healthcare and rehabilitation interventions, remains unclear. In our recently published book “COVID-19 and Parkinsonism” [6], we covered numerous aspects of COVID-19, parkinsonism, and PD from pathophysiology to treatment, emphasizing the need for high-quality research to disentangle possible pathophysiological mechanisms and long-term sequelae of the recent pandemic.
References
-
Leta V, Urso D, Batzu L, Lau YH, Mathew D, Boura I, Raeder V, Falup-Pecurariu C, van Wamelen D, Ray Chaudhuri K. Viruses, parkinsonism and Parkinson's disease: the past, present and future. J Neural Transm (Vienna). 2022 Sep;129(9):1119-1132. doi: 10.1007/s00702-022-02536-y.
-
Boura I, Chaudhuri KR. Coronavirus Disease 2019 and Related Parkinsonism: The Clinical Evidence Thus Far. Mov Disord Clin Pract. 2022 Apr 28;9(5):584-593. doi: 10.1002/mdc3.13461.
-
Antonini A, Leta V, Teo J, Chaudhuri KR. Outcome of Parkinson's Disease Patients Affected by COVID-19. Mov Disord. 2020 Jun;35(6):905-908. doi: 10.1002/mds.28104.
-
Leta V, Rodríguez-Violante M, Abundes A, Rukavina K, Teo JT, Falup-Pecurariu C, Irincu L, Rota S, Bhidayasiri R, Storch A, Odin P, Antonini A, Ray Chaudhuri K. Parkinson's Disease and Post-COVID-19 Syndrome: The Parkinson's Long-COVID Spectrum. Mov Disord. 2021 Jun;36(6):1287-1289. doi: 10.1002/mds.28622.
-
Leta V, Boura I, van Wamelen DJ, Rodriguez-Violante M, Antonini A, Chaudhuri KR. Covid-19 and Parkinson's disease: Acute clinical implications, long-COVID and post-COVID-19 parkinsonism. Int Rev Neurobiol. 2022;165:63-89. doi: 10.1016/bs.irn.2022.04.004.
-
Ray Chaudhuri K, Rodriguez-Violante M, Antonini A, Boura I. Covid-19 and Parkinsonism. Int Rev Neurobiol. 2022. 165.
Read more Moving Along: